Suicide in the U.S. is a Growing Public Health Issue
Suicide can be viewed as a process that begins with suicidal ideation, followed by planning and then by a suicidal act, and suicidal ideation can be prompted by depression or PTSD

1. Owens PL (AHRQ), Fingar KR (IBM Watson Health), Heslin KC (AHRQ), Mutter R (SAMHSA), Booth CL (SAMHSA). Emergency Department Visits Related to Suicidal Ideation, 2006-2013. HCUP Statistical Brief #220. January 2017. Agency for Healthcare Research and Quality, Rockville, MD. http://www.hcup-us.ahrq.gov/reports/statbriefs/sb220-Suicidal-Ideation-ED-Visits.pdf.
2. Center for Behavioral Health Statistics and Quality. (2020). Results from the 2020 National Survey on Drug Use and Health: Graphics from the Key Findings Report - Rockville, MD: Substance Abuse and Mental Health Services Administration. Retrieved from https://www.samhsa.gov/data/sites/default/files/reports/rpt35325/2020NSDUHFFRSlides090821.pdf. Accessed December 7, 2022.
3. CDC Suicide Prevention: Suicide Data and Statistics. Available at: https://www. https://www.cdc.gov/suicide/suicide-data-statistics.html/. Accessed September 6, 2023.
Suicide rates saw a 37% increase between 2000-2018 and began to rise again in 2021
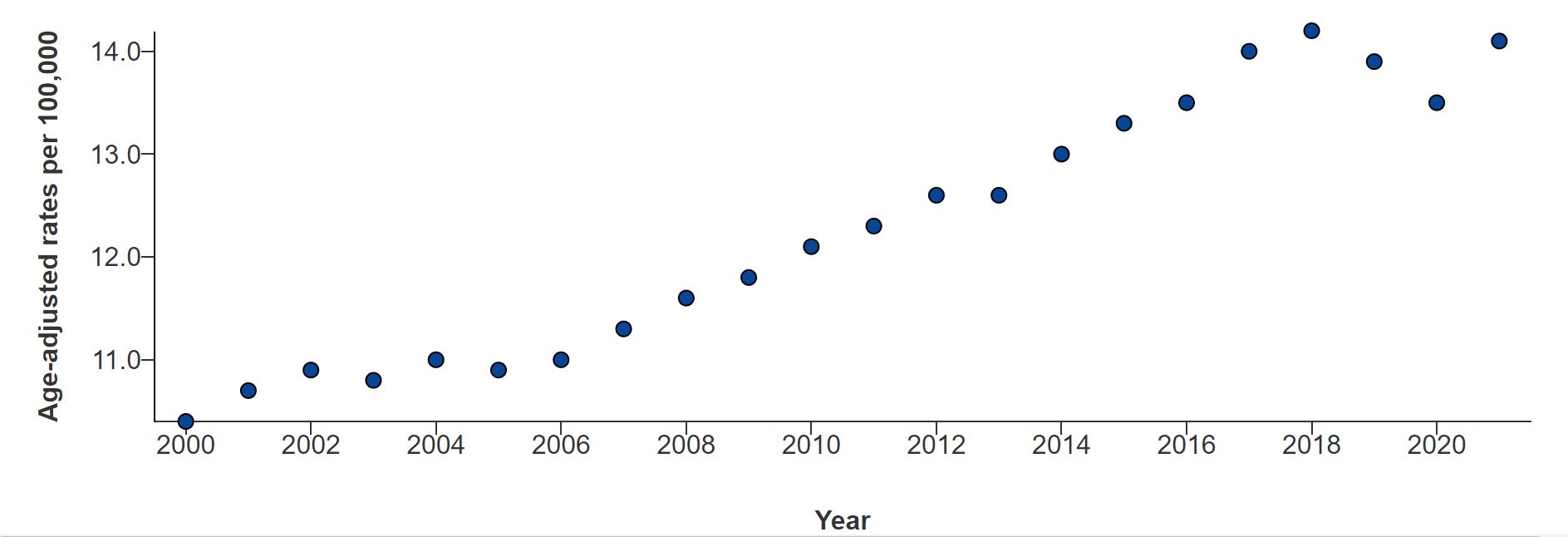
1. CDC Suicide Prevention: Suicide Data and Statistics. Available at: https://www. https://www.cdc.gov/suicide/suicide-data-statistics.html/. Accessed October 28, 2023.